Early Recognition and
Diagnosis of Ectodermal Dysplasia
What to Look For in Your Patients
There are about 150 different types of ectodermal dysplasia, each of which are genetic conditions affecting the development of skin, teeth, hair, nail, exocrine and sebaceous glands. Hypohidrotic ectodermal dysplasia (HED) is the most common form of ED, and the vast majority of HED cases are the X-linked form (XLHED) – 95% of males with HED have XLHED.1
Clinical diagnosis of XLHED is typically based on the triad of hypo- or anhidrosis, oligo- or anodontia and hypotrichosis,2 and genetic testing is available. Many medical specialties may have an important opportunity for diagnostic suspicion – including dentists, dermatologists, general practitioners, and their pediatric counterparts, as well as obstetricians/gynecologists, geneticists, and genetic counselors.
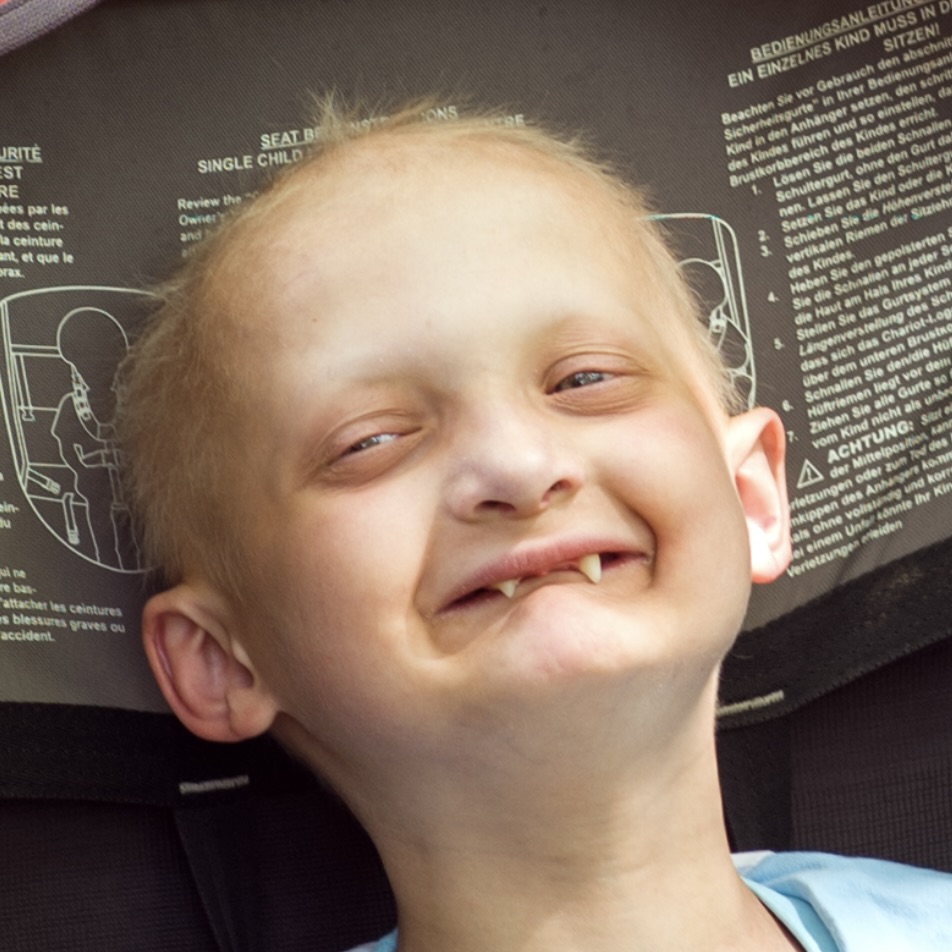
Clinical Characteristics
- Hair: scalp hair is frequently blonde, fine, and short; eyebrows and eyelashes are frequently missing
- Teeth: oligodontia requiring dentures or dental implants
- Skin: smooth, dry and thin, with fine wrinkles and increased pigmentation present around the eyes and mouth
- Immune/Respiratory: increased susceptibility to asthma, eczema and sinusitis; chronic, foul-smelling nasal discharge

Female Heterogeneity
Though the clinical spectrum is fully expressed in affected males, females are heterozygous and present with more heterogeneous and often less severe phenotypes. Natural history suggests that ≥50% of females with the XLHED mutation have signs or symptoms that can be detected through interview and clinical examination, including:2
- 99% have family history of XLHED
- 75% have reported sweating abnormalities
- 73% have missing permanent teeth (often first sign for female diagnosis)
- 26% have reported family history of infant/childhood deaths
- Aplastic or hypoplastic mammary glands1
XLHED Genetics
XLHED Genetics
Every patient affected by XLHED has a 50% chance of passing the mutation to their children. As with other X-linked disorders, males with the mutation have a fully affected phenotype, while females are heterozygous and have a variable phenotype.
If you suspect XLHED in any of your patients, they may wish to contact an ectodermal dysplasia patient advocacy group for genetic testing. Women with the XLHED mutation who are pregnant or planning for pregnancy may be eligible for the Edelife clinical trial.
XLHED Inheritance (X-linked)
Example: mother carries XLHED mutation to son

X, Y = unaffected genes
Because of X-linked genetics, boys inheriting XLHED from their mother are most likely to be fully affected

NEXT STEPS: EDELIFE STUDY ENROLLMENT
Early suspicion and referral are essential. Contact an Edelife clinical site to refer a patient or request more information.
References: 1. Deshmukh S, Prashanth S. Ectodermal Dysplasia: A Genetic Review. Int J Clin Pediatr Dent 2012; 5(3):197-202. 2. Fete M, Hermann J, Behrens J, Huttner KM. 2014. X-linked hypohidrotic ectodermal dysplasia (XLHED): Clinical and diagnostic insights from an international patient registry. Am J Med Genet Part A 164A:2437–2442. 3. Körber, I.; Klein, O.D.; Morhart, P.; Faschingbauer, F.; Grange, D.K.; Clarke, A.; Bodemer, C.; Maitz, S.; Huttner, K.; Kirby, N.; et al. Safety and immunogenicity of Fc-EDA, a recombinant ectodysplasin A1 replacement protein, in human subjects. Br. J. Clin. Pharmacol. 2020, 86, 2063–2069.


